 Whispers in the library are deafening. The piles of books are staring back at you as if they are mocking you. The weekend is almost here though and your exam is just six hours away. This is the final push to learn everything before exams. You have been trying to study, but distractions are constant and are ruining the ability to really cram the knowledge you need. Too often in the United States, this exact scenario will lead to a young adult or teenager turning to a medication that has not been prescribed to them as a way to cope with the lack of focus. Most of those times it is Adderall that is turned to. Still buzzing from the doses of Adderall taken, you take your exams and it’s time to let loose with your friends and classmates with social drinking for the weekend. While using Adderall as prescribed and in the right dosage, like drinking alcohol in moderation, may not have long lasting effects on the mind and body, there can be damage as a result of using both simultaneously. As the two substances are negating each other’s actions on the body, the two battle back and forth as you feel dampened effects from each. So you have to take more to rebound. The cycle has begun.
Whispers in the library are deafening. The piles of books are staring back at you as if they are mocking you. The weekend is almost here though and your exam is just six hours away. This is the final push to learn everything before exams. You have been trying to study, but distractions are constant and are ruining the ability to really cram the knowledge you need. Too often in the United States, this exact scenario will lead to a young adult or teenager turning to a medication that has not been prescribed to them as a way to cope with the lack of focus. Most of those times it is Adderall that is turned to. Still buzzing from the doses of Adderall taken, you take your exams and it’s time to let loose with your friends and classmates with social drinking for the weekend. While using Adderall as prescribed and in the right dosage, like drinking alcohol in moderation, may not have long lasting effects on the mind and body, there can be damage as a result of using both simultaneously. As the two substances are negating each other’s actions on the body, the two battle back and forth as you feel dampened effects from each. So you have to take more to rebound. The cycle has begun.
A is For Adderall and The Grades We Hope To Have
Chances are that if you are between the ages of 15-35 in the United States in 2020, you have come across someone misusing Adderall and there is a chance that you have done it yourself as it becomes more mainstream over time. Typically used as a medication for Attention Deficit Hyperactivity Disorder, commonly referred to simply as ADHD, Adderall addiction cases and emergency room visits have risen in recent years, particularly among those in the 15-25 years old age bracket. Most commonly, when misused, the drug is obtained not through a prescription, but through an acquaintance that has a prescription. The Drug Enforcement Agency lists Adderall as a Schedule II drug, meaning there is a high potential for misuse and it can lead to dependence both physically and psychologically.  As with any drug, use over time can have side effects a mile long. Perhaps you have found yourself in an exam in Roethke Auditorium or The Cue and after taking an Adderall you cannot stop shaking. Your mind starts racing as to what is wrong with you and you can no longer focus on the rest in front of you. Turns out, what you’re experiencing is a common side effect of Adderall. The side effects include:
As with any drug, use over time can have side effects a mile long. Perhaps you have found yourself in an exam in Roethke Auditorium or The Cue and after taking an Adderall you cannot stop shaking. Your mind starts racing as to what is wrong with you and you can no longer focus on the rest in front of you. Turns out, what you’re experiencing is a common side effect of Adderall. The side effects include:
- Restlessness
- Shakiness
- Headaches
- Stomach pain
- Weight loss
- Changes in sex drive
- Diarrhea
- Insomnia
- Anger/irritation
- Hallucinations/delusions
The more serious side effects include:
- Chest pain
- Heart arrhythmia
- Shortness of breath
- Numbness in the body
- Seizures
- Swelling of face/tongue/throat/eyes
- Slowed/slurred speech
- Rashes and hives.
Using Adderall for ADHD and its Effects
Over time, Adderall has become a household name in the United States as it is one of the most commonly prescribed stimulants across the board. In cases of medicating ADHD, the drug has been known to be quite effective — its success also plays into the reason it is commonly misused though. Stimulants frequently referred to as uppers, are invigorating and pleasurable in their effect on the mind and body. They can increase confidence, attentiveness, and functionality to give the user a feeling of success. Specifically, with Adderall, prescribers use it as an effective way of managing ADHD symptoms such as short attention span, impulsive behavior, and hyperactivity. They may be used alone or in combination with behavioral therapy. According to the Cleveland Clinic, stimulant drugs, such as Adderall, improve ADHD symptoms in about 70 percent of adults and 70-80 percent of children shortly after starting treatment. Improvements from the medication include reduced interrupting, a reduction in fidgeting, and other hyperactive symptoms, as well as improved task completion and home relationships.  Adderall is often quick to begin working in all individuals that take it, either in capsule or extended-release tablets. Due to the fact that there is not a diagnostic test for ADHD, many see issues with over-prescribing of Adderall. A diagnosis of ADHD requires the use of medical, psychological, social, and educational resources. A diagnosis can be made based on a simple evaluation of the patient. Improvements in behavior and attention span usually continue as long as the medication is taken, although benefits in social adjustment and school performance have not yet been shown to endure over the long term.
Adderall is often quick to begin working in all individuals that take it, either in capsule or extended-release tablets. Due to the fact that there is not a diagnostic test for ADHD, many see issues with over-prescribing of Adderall. A diagnosis of ADHD requires the use of medical, psychological, social, and educational resources. A diagnosis can be made based on a simple evaluation of the patient. Improvements in behavior and attention span usually continue as long as the medication is taken, although benefits in social adjustment and school performance have not yet been shown to endure over the long term.
A Is For Alcohol Too…
Studies have shown that as many 10.6 percent of students in universities are using Adderall or another form of non-prescribed stimulant in a given school semester. Of that 10.6 percent of students that were using non-medically prescribed stimulants, an astounding 46.4 percent of them were also drinking alcohol at the same time. While students often take these stimulants for help in coursework throughout their college career, the study also found that these students that were taking stimulants that were not prescribed to them and drinking alcohol simultaneously were earning lower grade point averages. It also found to be true that these students were using more substances than just stimulants and alcohol, as well as increased alcohol-related consequences. 
Dangers of Alcohol
Alcohol is the most commonly used drug in the United States. It is sold in stores across the country in quantities of millions of dollars on a daily basis. As alcohol remains readily available at almost every store, the dangers of possible misuse remain strong. According to the National Institute on Alcohol Abuse and Alcoholism (NIAAA), more than 85.6 percent of people ages 18 or older reported that they drank alcohol at some point in their lifetime; 69.5 percent reported that they drank in the past year; 54.9 percent reported that they drank in the past month. Furthermore, alcohol use disorder (alcoholism) stats remain steady in the eight figures. According to NIAAA, 14.1 million adults ages 18 and older had AUD. This includes 8.9 million men and 5.2 million women.
The Facts and Stats on Alcohol Use in Universities
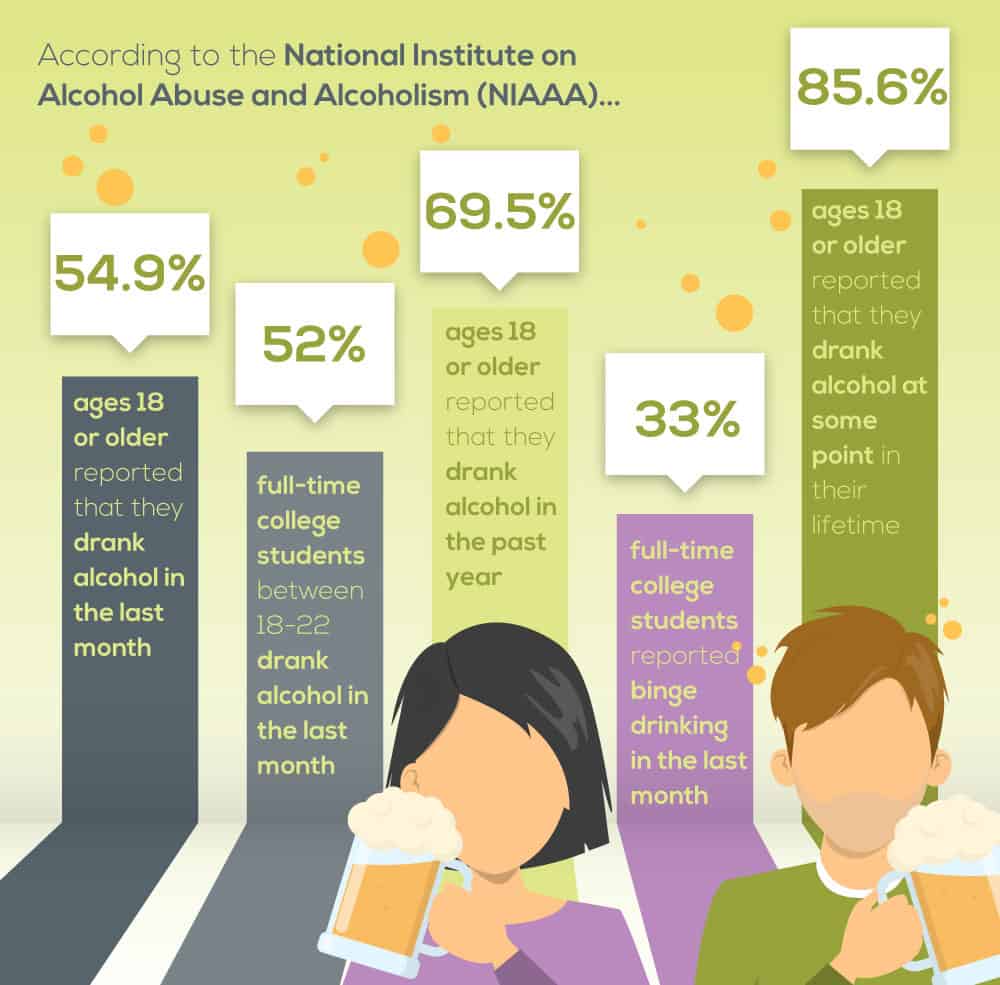 Thousands of Huskies and Cougars alike have found themselves at a crossroads with alcohol at some point during college. Oftentimes, a friend or roommate is having some friends over for some drinks. Those drinks may be leading into more drinks and eventually into a night that cannot be remembered. Research from the NIAAA indicates that as many 52 percent of full-time college students between the ages of 18 and 22 drank alcohol within the past month. That is an 8 percent increase to fellow young adults between 18-22 that had a 44 percent rate of drinking in the past month. Thirty-three percent of students reported binge drinking in the past month. Roughly 9 percent of students met the criteria for AUD. Around 25 percent of college students face academic problems due to drinking alcohol, according to the NIAAA study.
Thousands of Huskies and Cougars alike have found themselves at a crossroads with alcohol at some point during college. Oftentimes, a friend or roommate is having some friends over for some drinks. Those drinks may be leading into more drinks and eventually into a night that cannot be remembered. Research from the NIAAA indicates that as many 52 percent of full-time college students between the ages of 18 and 22 drank alcohol within the past month. That is an 8 percent increase to fellow young adults between 18-22 that had a 44 percent rate of drinking in the past month. Thirty-three percent of students reported binge drinking in the past month. Roughly 9 percent of students met the criteria for AUD. Around 25 percent of college students face academic problems due to drinking alcohol, according to the NIAAA study.
Mixing It Up: Alcohol and Adderall
In general, mixing stimulants with other substances, especially depressants such as alcohol, can be harmful, as they all have different effects on the body. By mixing the two, you are confusing your body with two differing effects hitting it simultaneously. Adderall, when entering the body, will speed up reflexes, heart rate, and breathing. It can enhance alertness, concentration, and reaction time. As alcohol enters the system, it produces feelings of calmness and sedation. Since it is a depressant, it can depress the central nervous system and slows heart rate and breathing. It can dull judgement, alertness, concentration and reaction time. Simply mixing the two can cause mass confusion to the body and mind as they battle. Because your mind takes on the effects of each, your judgement can be dampened, leading to the urge to overcompensate as feelings from each are dulled. People mix alcohol and stimulants for many reasons. Some drink in an attempt to improve their feeling of euphoria from the stimulants. Others might be trying to take the edge off from the stimulant they are experiencing a high from. Sometimes, a person might be taking a stimulant to come out from the tiredness brought on by alcohol consumption. Regardless of the reason for combination, it is dangerous. As you feel the dampened effects from Adderall altering consuming alcohol, you might find yourself taking more to overcome. This often leads to an overdose. In the same way, not feeling the normal effects of alcohol after taking Adderall, might lead to drinking more. This leads to alcohol poisoning. Both can be deadly and both are unfortunately likely when a person combines the two as judgement and decision making are both altered significantly by both substances. As decision making and judgement are altered by use of both of these substances, it becomes harder for the person battling a substance use disorder to realize there is an issue and treatment must be sought.
Medical Detox and Addiction Treatment for Adderall and Alcohol
Recovering from a physical or psychological dependence on alcohol and recovery from a physical or psychological dependence on Adderall are both difficult. Recovering from both simultaneously is even harder. Many people believe that quitting cold turkey is the answer, while others might turn to a natural detox method to get through. Some even believe that you can taper yourself off of a drug slowly to lessen withdrawal symptoms. None of these are recommended. Going through a medical detox from alcohol and/or Adderall addiction is proven to be the most effective way to begin treatment. While the first step may involve a medical taper, you will be treated with medical professionals overseeing you through each step of the detox phase in recovery. Having doctors and other professionals present while the body recovers, will reduce the risks that come with withdrawal. Many ask whether medical detox or drug rehab are better, when the answer is both. Entering rehab treatment without detoxing first can lead to an unsuccessful attempt at recovery, as your body is still full of the substance-related toxins. The period of detoxing allows for the patient to enter treatment with a clear mind to focus entirely on treatment and finding the root of their addiction. At the same time, going through detox, while great for the mind and body, will not be enough in most cases to carry over to long-term recovery. This is why we suggest that it is best to do both.
Treat Your Addiction At Northpoint Washington
Following a period of detoxification, it is essential that an addicted individual enter rehab for treatment. At this point, recovery truly begins and opens the possibility of long-term recovery. Without this step, it is possible an addicted individual will return to substance dependence and misuse. In rehab, the goal is to reach the heart of the addiction. By finding the causes, a person can better understand the factors that lead to substance use in the first place. Generally, using modalities of treatment such as group therapy, dual diagnosis, medical intervention, family therapy, psychiatric care, meditation, relapse prevention and more, patients will gain a stronger understanding of the root of their substance use and know the triggers as they happen. At Northpoint Washington, patients receive top of the line care in our outpatient programs, designed to rid the body of dependence and begin the journey to a long-term recovery. If you or a loved one are battling the issue of mixing alcohol and Adderall, call 425.437.3298 today for assistance.

