“We are seeing more people killed because of opioid overdose than from traffic accidents – I mean, think about that. It has to be something right at the top of our radar screen.” ~ President Barack Obama, speaking at the 2016 National RX Drug Abuse and Heroin Summit Drug overdose is the leading cause of accidental death in the United States – 47,055 people died because of lethal drug overdoses in 2014. And the majority of those deaths can be traced back to opioids – prescription painkillers like OxyContin or Vicodin or the illicit street drug heroin. 
Opiate Statistics in the United States
The Centers for Disease Control and Prevention have referred to the opioid “epidemic” in the United States, and the latest data shows that the term is no exaggeration: 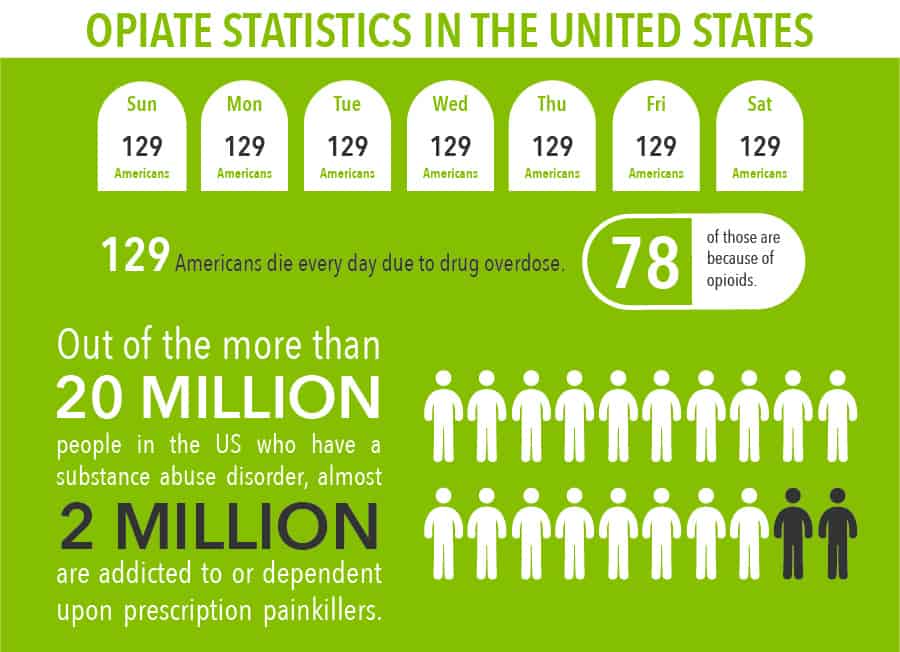
- 129 people Americans die every day due to a drug overdose – 78 of those are because of opioids.
- Out of the more than 20 MILLION people in the US who have a substance abuse disorder, almost 2 MILLION are addicted to/dependent upon prescription painkillers and another 586,000 have a problem with heroin.
- Among the overdose deaths are 18,893 due to prescription pain relievers and 10,574 because of heroin.
- Since 1999, deaths from prescription opioids – methadone, hydrocodone, oxycodone, etc. – have quadrupled.
- It is estimated that the number of emergency room visits involving opioids is five times the number of deaths.
- In 2009, the rate of new treatment admissions related to opioids was six times what it was in 1999.
How Do Opioids Kill?
Opioid medications are dangerous, because the amount needed to alleviate pain and the amount that is potentially deadly is very small, and often, unpredictable. The stronger a medication is, the smaller the margin of error becomes – sometimes, life and death are separated by micrograms. The #1 hazard associated with opioids like prescription painkillers and heroin is respiratory depression – slowed or stopped breathing. This effect is extremely pronounced when the opioid is taken with certain other substances, such as:
- Alcohol
- Sleeping pills
- Antianxiety medicine
- Other opioids
For example, if a person who is drinking takes a pain pill, they are at extreme risk of passing out, stopping breathing, and dying – even if they have only taken the proper dosage of their medication. Extended-release opioids like methadone are particularly dangerous because their pain-relieving qualities (or, if used recreationally, their euphoric effects) will wear off before their tendency to suppress breathing does.
Tolerance Increases the Risk of Overdose
Tolerance is when a person’s body has become accustomed to the drug and takes ever-increasing amounts to achieve the same effect. In other words, a person who has been using opioids (or any other substance) will, after a time, feel less of the effect than would a new user. The pain relief and the recreational high aren’t as significant as they were in the past. So, they take more. But, there is much less tolerance for the respiratory effects of opioids. This is one of the most frequent causes of an opioid overdose – the user/abuser wants to relieve their pain or experience a high, but their dosage has reached the point where their breathing stops. There is also evidence to suggest that long-term consumption of opioids can actually worsen a person’s perception of pain – a condition called hyperalgesia. This creates a self-perpetuating cycle of increasing pain, leading to increasing opioid consumption, leading to increased pain.
Why Relapse after Recovery Can Be Deadly
Most people who develop an opioid dependence or addiction do try to get clean. Unfortunately, their first efforts are usually to quit on their own, cold-turkey. Because of the changes in the brain caused by addiction, they are almost certainly doomed to failure. It isn’t a matter of choice or willpower – they are held hostage by the compulsions of addiction. These compulsions can be strong enough to even make some people relapse – go back to using drugs – early on during the treatment process. But relapsing after a period of sobriety can be fatal for opioid abusers. The first thing that has to happen before recovery can begin is opioid detoxification – a period of abstinence, usually lasting anywhere from a few days to a few weeks. During this time, the body physically purges itself of the opioids. It can be a harshly unpleasant experience for opioid abusers as they endure withdrawal symptoms:
- Heightened anxiety
- Irritability
- Depression
- Bodily tremors
- Muscle cramps and aches
- Flu-like symptoms
- Vomiting and diarrhea
- Extreme drug cravings
When the opioid detox process is finished, the person is virtually free of the physical compulsion to use drugs, and they can then truly begin the recovery process. But the psychological dependence still exists at this point, this is when the danger of relapse can turn deadly. When a person who has been sober for any length of time resumes drug use, they invariably go back to using the same amount they had been before abstinence. But here’s the problem – The detox process and/or the period of sobriety has removed much of that person’s tolerance for opioids. They take their accustomed-to dosage and are overwhelmed. In other words, a newly-sober-but-relapsing opioid abuser can suffer a fatal overdose even if they use their “normal” amount.
So What Can Be Done to Lessen the Chances of an Opioid Overdose?
Obviously, the best way to protect yourself against an opioid overdose is never to misuse opioids in the first place. If you need a prescription to manage your pain, you should start by having an open and honest conversation with your physician about alternatives to opioids. And, if you or someone in your family has a history of substance abuse, you need to bring that fact up to your doctor, so you can avoid being prescribed drugs that may jeopardize your sobriety. Follow your doctor’s instructions, because there are many pain management options available to you – weight loss, diet, massage, physical therapy, exercise, etc. If you are already dependent on or addicted to prescription painkillers or heroin, then you should not attempt to get clean by yourself. Avail yourself of the services of a local opioid detox facility and both medical supervision and medication assistance to make sure that you are safe and supported during the detox process. Likewise, don’t try to abstain from intoxicants all by yourself. Your chances for a successful return to sobriety greatly depend upon the support and structure you get from a professional evidence-based drug rehab program, 12-Step meetings, and your friends and family members.
Full Infographic:
 SOURCES: https://www.cdc.gov/drugoverdose/epidemic/index.html https://www.asam.org/docs/default-source/advocacy/opioid-addiction-disease-facts-figures.pdf https://www.nytimes.com/2016/03/30/us/politics/obama-steps-upus-effort-to-fightabuse-of-heroin-and-painkillers.html?_r=0 https://www.latimes.com/nation/la-sci-sn-opioid-overdose-prescription-hospital-er-20141026-story.html
SOURCES: https://www.cdc.gov/drugoverdose/epidemic/index.html https://www.asam.org/docs/default-source/advocacy/opioid-addiction-disease-facts-figures.pdf https://www.nytimes.com/2016/03/30/us/politics/obama-steps-upus-effort-to-fightabuse-of-heroin-and-painkillers.html?_r=0 https://www.latimes.com/nation/la-sci-sn-opioid-overdose-prescription-hospital-er-20141026-story.html


