Location
Our Washington Location
Our inpatient facility is located in Washington, and will serve Washington state. It will provide a safe & therapeutic environment for both our staff and patients.
- Edmonds
7416 212th St SW,
Edmonds, WA 98026


Disclaimer: This article is not intended as a substitute for the counsel of a qualified physician or licensed therapist. This content should be used for purely informational purposes. Please consult your doctor if you have further inquiries on this subject. We intend to impart the most accurate and recent information but cannot make any guarantees.
Some call it a modern miracle or even an answer to the opioid epidemic. Others call it an addiction in disguise. For those searching for help with substance abuse or opioid addiction, it can be hard to decide who to believe. So what's the deal, is Suboxone a miracle or a crutch? Good or evil?

"Withdrawal wasn't a painful process for me with Suboxone. You just feel normal. It has worked really well for me." -- Mike Sorrentino "The Situation" of Jersey Shore
Some celebrities who have suffered from substance use disorder, such as Jersey Shore's Mike "The Situation" Sorrentino or '90s TV star Kristen Johnston, give Suboxone full credit for their recovery. Both stars were addicted to prescription opioids and both were prescribed Suboxone as treatment for their addictions. They are still sober today.


Due to so many stories like those above (as well as piles of research), thousands of doctors and accredited drug rehab centers advocate the use of medications like Suboxone to help people with opioid use disorder achieve sobriety.
Then you have other addiction specialists and trusted 12-step abstinence programs that heartily contest the use of medications for the purpose of addiction treatment. This is an excerpt from a Narcotics Anonymous pamphlet:
"We make a distinction between drugs used by drug replacement programs and other prescribed drugs because such drugs are prescribed specifically as addiction treatment. Our program approaches recovery from addiction through abstinence, cautioning against the substitution of one drug for another."
If you are currently analyzing the best possible addiction treatment options for you or someone you care about, mixed opinions like these can be confusing, even distressing. So what's the truth? Is Suboxone an appropriate treatment for opioid dependency, or is abstinence the best way? In this article we'll explore the use of Suboxone as addiction therapy - its benefits, its dangers, and its own potential for dependency.
Suboxone is a brand name medicine prescribed to reduce drug withdrawal symptoms and cravings in association with opioid addiction. Suboxone is one brand name, although the drug is also available under the name Zubsolv. The medication combines two different substances:


Buprenorphine - A synthetic opioid that is only a partial-agonist, meaning that it does not produce the same level of euphoria as full-agonist opioids, but does stimulate the same receptors in the brain.
Naloxone - A substance that blocks opioid receptors in the brain, inhibiting all the effects of opioids, including any potential euphoric high. It can also cause an opioid user to go into full drug withdrawal if mixed with full-agonist opioids.
If these two substances sound like exact opposites, it's because they are. Both of these drugs bind to opioid receptors in the brain and work to cancel out the undesirable effects of the other. In other words, the buprenorphine can prevent naloxone from causing withdrawal symptoms while the naloxone can prevent buprenorphine or any other opioid from causing the user to experience a pleasurable "high".
When taken together, as with Suboxone, buprenorphine and naloxone can trick your brain into thinking it is receiving the opioids it craves, effectively staving off withdrawal symptoms while blocking the euphoric effects of any opioid the user takes. It sounds like the perfect solution, right? It's true that Suboxone is effective - almost too effective. The drug makes chronic drug users feel so functional that they may continue to take the medication for far longer than necessary, creating a new dependence. Such is the dilemma with Suboxone, which we'll explore further in the sections below.
Now that you've got some basic definitions, we can delve into the true objective of Suboxone - to soothe withdrawal symptoms and discourage opioid abuse during addiction recovery. These attributes make the drug an effective part of medication-based drug treatment protocols, like opioid replacement therapy (ORT) or medication-assisted treatment (MAT). This is how it works:


For the purposes listed above, Suboxone works remarkably well as part of a drug treatment program. The medication can be used to help you to wean yourself off of opioids without going through the worst symptoms of withdrawal, in addition to a much lower chance of relapsing during detox. It is not ideal as a long-term solution, however. Long-term use of Suboxone can have disastrous consequences.
Currently the only way to administer the medication is to place a Suboxone film strip under the tongue until it dissolves. Other generic alternatives are administered in much the same manner.

Suboxone should only be obtained by a prescription from a certified Suboxone doctor with experience and training in addiction treatment. Such a doctor will have the expertise necessary to prescribe the precise dose needed to prevent withdrawal symptoms without creating a severe dependence. It is possible to prescribe up to 32mg per day of Suboxone for severe cases, but the necessary dosage is usually only 8mg to 16mg for most people. The lower the dosage at the start, the easier it will be to taper off of the drug.


A Suboxone maintenance program refers to the process of tapering off of Suboxone as you wean yourself off of opioid use altogether. It can be a complex process; a Suboxone maintenance program should be monitored carefully by a doctor to oversee side effects, reactions, and withdrawal symptoms. The dose should be just enough to keep away drug withdrawal but not so much that it causes heavy side effects. Too large of a dose, and the tapering process will be more difficult; too low of a dose, and the withdrawal symptoms will be more severe. The way that your Suboxone maintenance program is administered could make or break your recovery process.

The safest way to use Suboxone for drug treatment purposes is to plan the tapering process from day one. The medication is most effective and less habit-forming when it is used as part of a short-term detox program. Your Suboxone dosage will depend on the severity of your addiction to opioids. For more severe cases, a higher dosage of 24mg or more may be necessary to reduce opioid withdrawal symptoms, while other patients may only need 8mg per day.


A good Suboxone doctor can help you to formulate a plan tailored to your needs that tapers off the drug over time in the most comfortable way possible. Some programs recommend a faster program of reducing Suboxone every four days until you reach 0.5mg. This is a quicker route. If you start off on 8mg per day, the tapering would look something like this:
Start: 8mg, Day 5: 4.6mg, Day 9: 2.6mg, Day 13: 1.5mg, Day 17: 0.9mg, Day 21: 0.5mg
Once you've taken 0.5mg for several days, you should be ready to drop the meds altogether with minimal withdrawal symptoms.
For higher doses, the changes from one day to another would be more significant:
Start: 16mg, Day 5: 8.0mg, Day 9: 4.0mg, Day 13: 2.0mg, Day 17: 1.0mg, Day 21: 0.5mg
As you can see, each change is a little more impactful with a higher dose, making for more discomfort and withdrawal with each taper.

Others may be more suited to a longer route that reduces Suboxone intake by 25% every 10 days. Even on slower programs, you could experience significant withdrawal symptoms each time the dose is reduced, so the less you take, the less withdrawals you'll experience.
In other words, you should work with your doctor to start your maintenance program at the lowest possible dose of Suboxone so that the process remains as comfortable as possible.
Despite research that shows its effectiveness, there is a lot of criticism for MAT in the realm of addiction treatment methodologies. Many people ask, "How can one drug be better than any other?" or "Why would you use opioids to treat opioid abuse?" While the philosophy itself may seem strange, evidence shows that it works.


The reason it works is because opioid withdrawal is one of the most painful, physically and emotionally harrowing ordeals that you can go through.
If you've been through it, you know what we're talking about. The severity of opioid withdrawal symptoms and cravings is the most common reason for relapse. That's why finding a way to soothe and reduce symptoms and cravings can be the key to achieving sobriety. Especially for those who have suffered from chronic relapses time and time again, MAT can be the difference that ends the cycle for good. There are several ways to approach medicated addiction treatment:
Opioid replacement therapy (ORT) refers to any use of synthetic, low-intensity opioids to treat opioid addiction, cravings, and withdrawal symptoms. Suboxone and methadone are two common medications used in these programs. Many clinics offer ORT prescriptions without any additional support, allowing patients to manage their own recovery.
Medication-Assisted Treatment (MAT) is a broader spectrum of treatment that requires patients to undergo other drug treatment therapies and counseling in conjunction with addiction treatment prescriptions. The American Society of Addiction Medicine has produced multiple studies and surveys that show MAT to be more effective in long-term recovery methods than either ORT or traditional drug counseling on its own.
Some other therapeutic practices that may be combined with medication in an MAT program include:
Methadone is the most well-known of ORT medications; it is by far the oldest, with a history of addiction treatment going as far back as the 1970s. For a long time, methadone was the only option in ORT treatment settings. Because it is a synthetic opioid that does not create an intense euphoria when used as directed, it has long been considered a viable option in reducing opioid withdrawal symptoms.

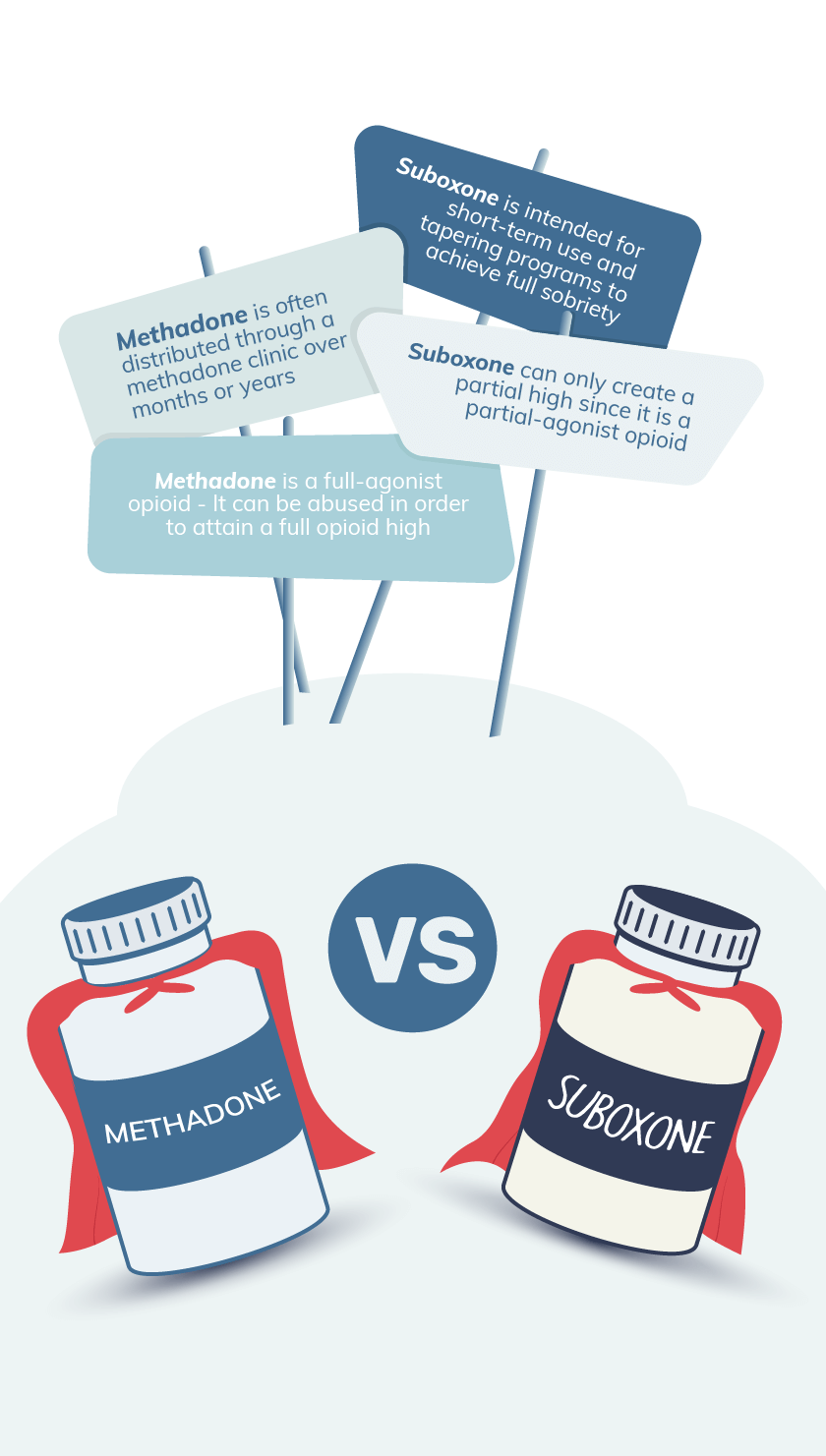
Unfortunately, methadone also a history of rampant abuse and overdoses among patients, which points to some major differences between methadone and Suboxone, such as:


As with most medications, side effects do not present in every patient, but these are possible side effects that may result from the use of Suboxone:


Suboxone does not play well with other meds. Even common, seemingly innocuous medicines like Tylenol and birth control can react badly with Suboxone, so it's important to tread carefully when taking any medications at all with Suboxone. Below we've listed the medications that are known to have negative drug interaction with Suboxone, but you should consult your prescribing doctor before taking Suboxone with any other meds at all:
Suboxone can certainly be addictive. The question of how addictive it is will depend on how the medication is used.


For example, many people take Suboxone exactly as directed by their doctor. Especially long-term opioid addicts will marvel at how they feel "normal" and "fully functional" for the first time in years. Although this is not the same as getting a drug-induced high, the sensation of normalcy can be seductive for someone who has struggled with the degradation of opioid abuse for years or decades. Some recovering addicts feel so good and productive when taking Suboxone that they have a hard time tapering off of it. The first sign of withdrawal symptoms at a dose change may send them running back to a higher dose. If this cycle continues, Suboxone use will continue long-term and dependence will form.
Of course, there are many people who do not take Suboxone as directed. Some patients increase their own dosage to much higher quantities than any doctor would recommend, hoping to achieve a buprenorphine high. Abusing Suboxone in this way will make the prescriptions run out faster, forcing users to buy the meds on the street. Consistent abuse will cause a strong dependence to form, making for a very difficult and painful tapering process.
Another form of abuse is to take Suboxone as a heroin dose in-between. Since Suboxone's qualities as a drug-withdrawal alleviator are well-known among opioid addicts, some choose to employ Suboxone as a way to stave off withdrawal symptoms when heroin is hard to find. Using Suboxone in this way is not only abusive, it also enables other more harmful addictions to subsist more easily.
Finally, the most severe form of Suboxone abuse is through intravenous injection. Because of the naloxone in the drug and its delivery as a sublingual film, abusing Suboxone is not always easy or successful. By dissolving the strips in water and injecting the resulting solution, however; some users have found a way around the manufacturers' attempts to prevent abuse. When taken intravenously, Suboxone is highly addictive and much more dangerous. Most overdoses of the medication have occurred in this way.
The short answer is yes, Suboxone can create a euphoric high when it is abused. The manufacturer has taken every precaution possible to prevent abuse of Suboxone, which is why it makes an ideal drug for addiction treatment. However, if it is taken in high doses or injected intravenously, Suboxone creates just enough of a high that it satisfies opioid cravings and the user's need for euphoria.


Suboxone does not create nearly the same level of euphoria as full-agonist opioids like heroin or hydrocodone, however; so it is often only used as a temporary fix in-between drug scores. It is important to note that if Suboxone is abused regularly, it will result in very severe withdrawal symptoms when the prescription runs out.
Compared to other opioids, Suboxone has a very long half life - about 24-42 hours. For this reason Suboxone's effects can last for two entire days, providing a respite from opioid withdrawal symptoms for much longer than other comparable medications.


Suboxone will stay in the blood or saliva for about 24 hours and in urine for 7 - 10 days. Many people on a Suboxone maintenance program worry about the drug showing up on obligatory workplace drug tests. Although Suboxone can show up in urine drug tests for up to 10 days, it will show up as buprenorphine, not as an opioid. With a note from your certified Suboxone provider, this shouldn't be a problem.
As we discussed earlier, Suboxone does not play well with others, and that includes illicit drugs or alcohol. Polysubstance abuse in any form is reckless and ill-advised, but with Suboxone it is truly dangerous.
First is the presence of naloxone in Suboxone that could have a quick and painful reaction to any illicit opioids or painkillers. If you mix naloxone with full-agonist opioids like heroin or oxy, the reaction of the two could make you feel like you've been suddenly thrown into the worst stage of drug withdrawal - vomiting, diarrhea, fever, the works.
There's also the more dangerous implication of mixing buprenorphine with other opioids. Since buprenorphine already slows down central nervous system processes like breathing and heart rate, throwing other opiods into the mix may double this effect, continuing to slow down the CNS until you collapse, overdose, or die outright.
The same is true of alcohol. Alcohol also slows down the CNS and all its processes. If you mix alcohol with buprenorphine, you are greatly increasing the chances that your body will forget to breathe. Double CNS depressants are always incredibly dangerous. The FDA has strongly advised Suboxone users to never mix it with alcohol.
Stimulants and club drugs are hardly advisable to take under any circumstances, but certainly not in conjunction with Suboxone. Cocaine and party drugs can block the effects of Suboxone, rendering it useless against the onslaught of opioid withdrawal symptoms. As a result, a hit of cocaine could result in instant drug withdrawal instead of a high. Buprenorphine can also cancel out the euphoric effects of stimulants, causing the user to take more and more in an attempt to get a buzz. This type of polysubstance cocktail can easily end in overdose without the user truly realizing how much they took.
Suboxone addiction is not always easy to recognize. Many patients assume that if the medication is doctor-prescribed and taken as directed, then it couldn't be a bad thing. Especially if Suboxone has been the solution that finally helped you to end a dangerous opioid addiction, long-term use of Suboxone may seem like a preferable, positive resolution. Unfortunately, if you've been taking the drug for months on end, it could be forming a dangerous dependence in and of itself.
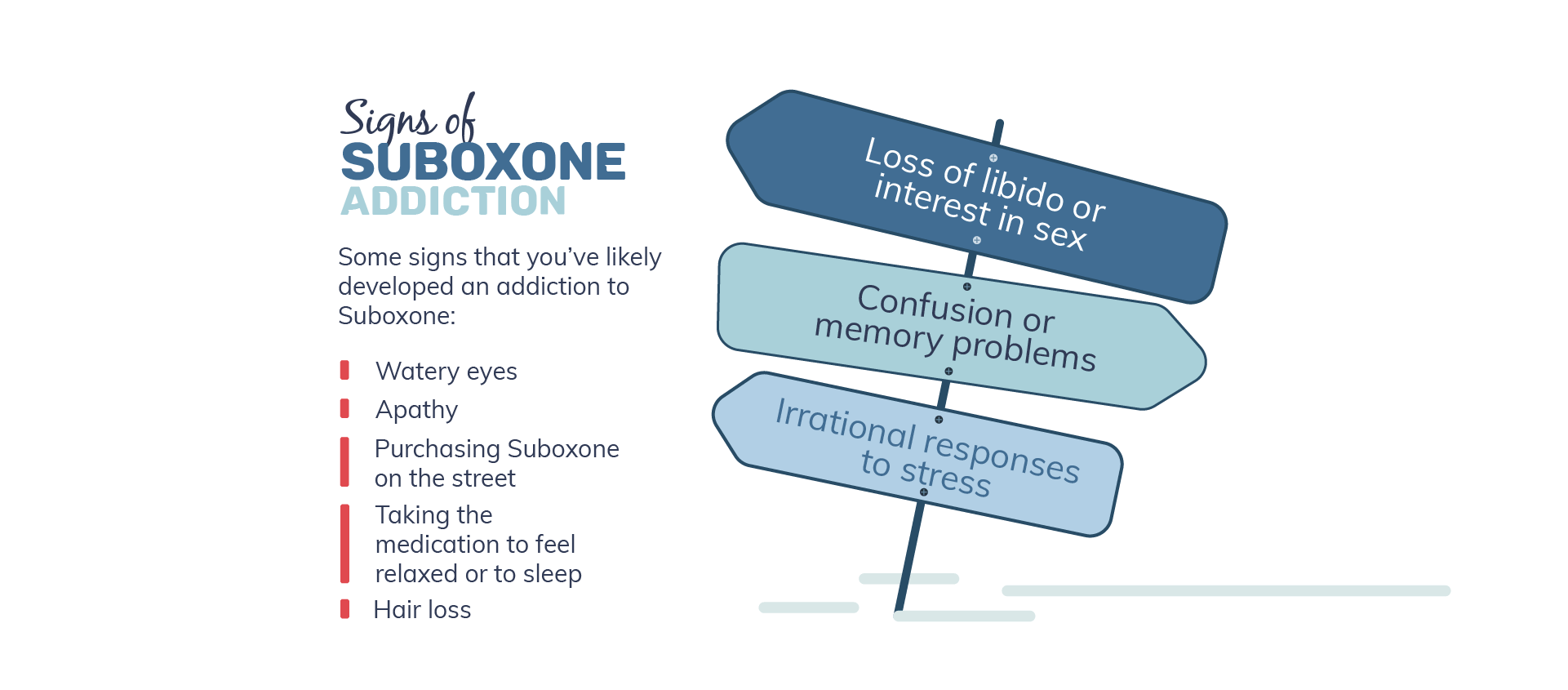
Of course, the first indicator of addiction is drug abuse. If you are using Suboxone in any way that was not recommended by your doctor - taking more than the recommended dose or shooting it up, for instance - then you already know that it's a problem.
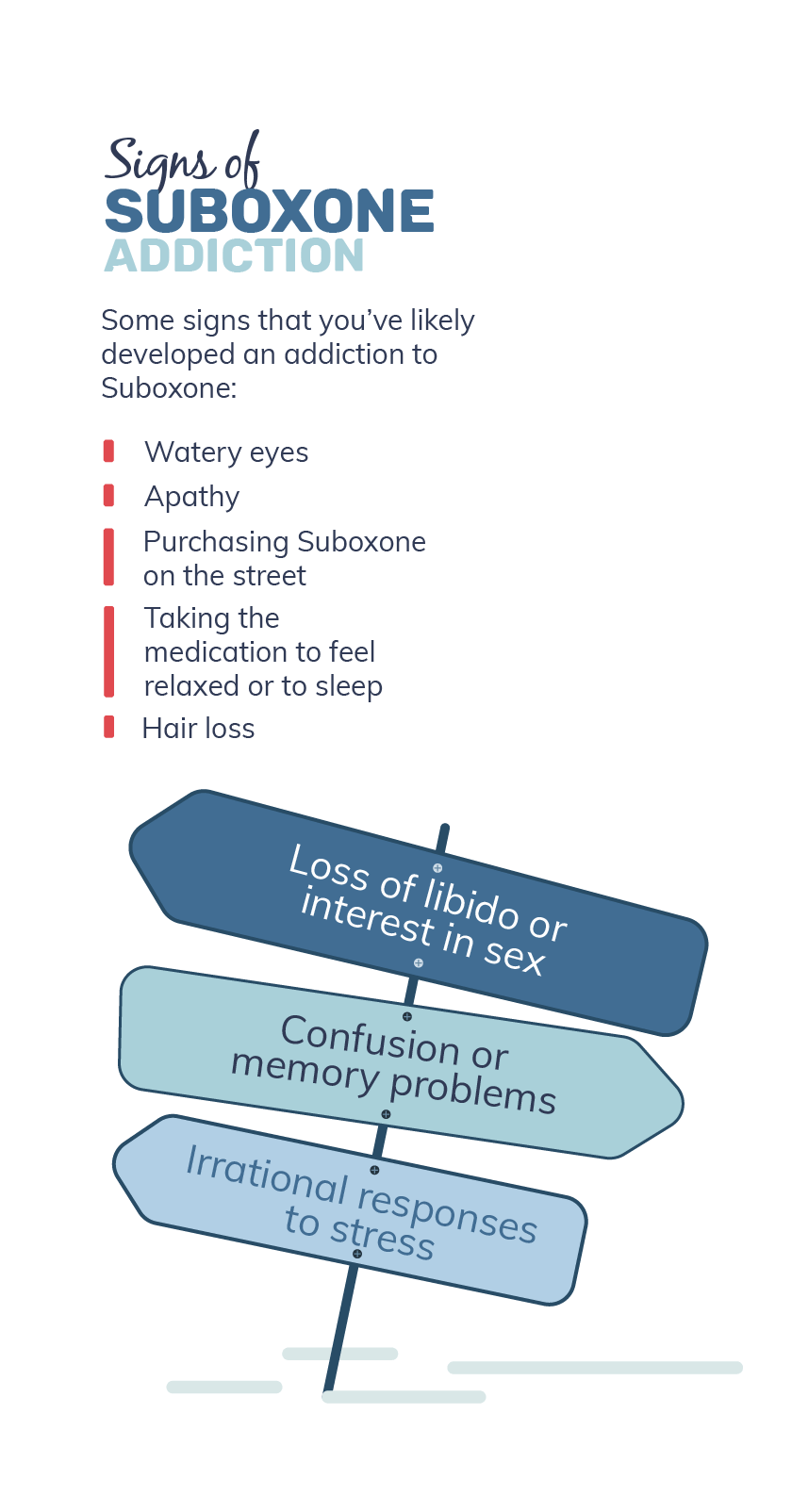
Other signs may be more subtle, like if you're having a very hard time tapering off of the medication. Here are some signs that you have likely developed an addiction to Suboxone:
Do you recognize any of these danger signs? If so, you are probably physically addicted to Suboxone. If this is the case, you should start formulating a safe tapering plan right away and find the help you need to manage the difficult process of recovery. Call an addiction hotline to get started today, or you can keep reading for more information on Suboxone addiction treatment.
Once a dependence to Suboxone has set in, the withdrawal symptoms you experience when you stop taking it can be even more serious than other opioids. Because of its long half-life, Suboxone withdrawal can be severe and long-lasting, especially if you try to quit "cold-turkey" instead of tapering off. Here is the Suboxone withdrawal timeline and its symptoms:


First 72 Hours
Day Four - Day Seven
Week Two - Week Four
Some of the psychological symptoms listed above could last for as long as two months, but most Suboxone withdrawal symptoms will fade by the second or third week. These symptoms may not look all that bad in list form, but when they are felt all at the same time, they culminate in a miserable, excruciating experience. If you are considering quitting Suboxone cold-turkey, consult with a licensed addiction care specialist first. The combined misery of the withdrawal symptoms listed above could easily lead to relapse. When the drug is tapered off slowly, withdrawal symptoms will be soothed and mollified, causing no more than a mild discomfort.

Perhaps you've tried to quit before. Relapse is painfully common and if you've been through the cycle of quitting, withdrawal, sobriety, and relapse; you may be ready to try anything to get clean for good. If you've tried the cold turkey method or other abstinence treatments only to relapse, MAT could be a fitting solution. Then again, you may have been told about the dangers of getting addicted to medications like Suboxone.
The danger is real. People do become dependent on Suboxone. That's why it's important to start MAT treatment with the intention of tapering down from the start, and always seek out the help of a licensed physician or addiction treatment center to supervise the process. Here are some patient tips to avoid becoming addicted to Suboxone during substance abuse treatment:
If you complete a carefully executed Suboxone maintenance program like the one described above, it is possible to safely detox off of opioids at a steady, controlled pace and achieve long-term recovery without long-term dependence on medication.
If you're reading this article because you have an existing Suboxone addiction, don't give up. Many excellent drug rehabilitation facilities offer complete programs to help patients taper off of Suboxone for good, even if the addiction has been going on for years. It is not an easy process; nor is it a quick one, but there are proven methods that work to help people create their own paths to long-term recovery. The first leg of the journey is drug detox.
Most people assume that the word "detox" means to abstain from all substances and medications cold turkey. However, we do not recommend a cold turkey approach for Suboxone because the withdrawal symptoms from this medication are particularly severe and long-lasting. Some symptoms may even pose a danger to your physical and emotional health.


A much more successful (and less excruciating) approach to Suboxone detox is a relatively high-speed taper that incorporates therapeutic activities to manage the resulting withdrawal symptoms. The severity and length of the addiction will determine how bad the withdrawal symptoms will be, but the experience will not be pleasant by any means. The key is to undergo a safe, medically supervised detox period with the best available treatments to ease the process.
Some effective Suboxone detox treatments include:

It may sound preferable to go through detox from the comfort of your own home, but this is not always advisable, especially in the case of Suboxone addiction. For one thing, many homes are full of triggers - drug paraphernalia, bad memories, and hard-partying roommates. Although you will eventually have to address all of these problems head-on, the detox period may not be the best time to face all of your demons.
Another problem with detoxing on your own is the sheer difficulty of the process. Suboxone addiction results in some of the worst-known drug withdrawal symptoms, and your home environment will not offer any of the medical supervision or therapeutic activities that can make the process safer and more bearable. Here are some reasons that most experts don't recommend undergoing Suboxone detox alone at home:
Just in case you missed that first fact, we cannot reiterate this enough:
Relapse during detox greatly increases your chances of overdose and death.
Relapse overdoses are the most common. This is because many drug abusers do not realize how quickly and dramatically tolerance can decrease during the first few days of detox. It often happens that patients begin the detox process with high hopes, managing to get through two or three days of sobriety before the withdrawal symptoms simply become too much. Then they relapse and take the exact same dose they were taking before. The problem with this is, their drug tolerance is much lower than it was a few days before, causing an instant overdose.
With some help to ease the terrible withdrawal symptoms, you will be much more likely to withstand those first crucial days of detox without relapsing. If you are determined to try detoxing from home, ensure that you can do it in the safest, least painful way possible. Ask your doctor to give you a full health examination beforehand to make sure you are physically healthy enough to undergo the process. Then, find an outpatient drug treatment center that can provide detox support with the right medications and outpatient treatments to help you through the process safely.
Many people think of "getting clean" as simply finding a way to quit using, but recovery is so much more. Even if you were to quit using Suboxone today, your sobriety wouldn't last long if you don't address the underlying causes of addiction. In order to achieve complete recovery and increase your chances of long-term sobriety, you must confront the psychological side of addiction. That is what drug rehabilitation is all about.


Many drug rehab facilities prefer to wait until the detox period is over before beginning rehab treatments, but since Suboxone tapering can be a long-term process, you will likely begin rehabilitation therapy while still undergoing the tapering process, as the dose become smaller and more manageable.
One of the most important goals of a good rehab program is to uncover the underlying causes of addiction. These may be hereditary, environmental, psychological, or any combination of factors. Many drug use disorders are the result of mental health conditions, so this will also be explored as a possible factor in your addiction. Once the primary contributing factors have been revealed, you can begin working with medical personnel and addiction counselors to analyze those thought patterns, attitudes, and behaviors that perpetuate drug abuse. With time and therapy, you can address the causes and contributors of your addiction and find healthier ways to channel those energies into a healthier, sober lifestyle.
Of course, it's not as simple as it sounds. There are many different therapeutic activities and treatments that contribute to this process. These are some of the key components of a comprehensive drug rehab center:

Dual Diagnosis - Over 60% of people with substance use disorder also suffer from other co-occurring mental health conditions. Dual diagnosis is a method of diagnosing those co-occurring disorders through a set of behavioral, emotional, psychological, and biosocial exams.
Integrated Treatment - Integrated treatment is the second phase of dual diagnosis - the practice of treating both addiction and mental health disorders at the same time. Through integrated treatment, clinicians hope to help you learn how to manage both conditions and build a functional lifestyle.
MAT - Medication assisted treatment is used to support both detox and rehabilitation programs. This could incorporate an assortment of pain management, ORT, or psychiatric meds to facilitate long-term recovery.
Relapse Prevention - Dealing with cravings and avoiding relapse will become part of daily routine in recovery. Rehab can help you learn how to manage these obstacles for the long-run.
Behavioral Therapy and Counseling - Clinically proven treatments like cognitive behavioral therapy, contingency management, and individual counseling with addiction therapists are integral to successful rehabilitation treatment.
Family Therapy - Families are complicated. Recovery may require you to mend broken relationships, explore family bonds, or even hash out difficult family histories. Building a family support system may be the major difference that helps you achieve long-term sobriety.
Group Therapy - Telling your own story and listening to stories about other people's battles is a natural part of the recovery journey. Process groups can help you consider your own history from a more objective point of view.
Holistic Activities - From exercise and meditation to nutrition, your whole-self wellness is vital to your emotional and physical health, in addition to your future. These activities are also important ingredients to a healthy lifestyle in recovery.
If you've read this far, it is safe to assume that you or someone you know has an addiction to Suboxone. Whether it's drug abuse or a long-term treatment plan that hasn't been managed well, Suboxone addiction can be detrimental, even dangerous, to your physical and emotional health. Unfortunately, it can be a very difficult habit to kick. The longer the addiction lasts, the harder it will be to stop.
Are you ready to put an end to Suboxone dependence? There's no reason to go it alone. Call our addiction hotline now to find out more about Suboxone detox and rehab options in your area. All it takes is a phone call. Let tomorrow be your Day One.

Our admissions coordinators are here to help you get started with treatment the right way. They'll verify your health insurance, help set up travel arrangements, and make sure your transition into treatment is smooth and hassle-free.
888.450.2153Contact Us